Institute: University of Oxford
Exploring mechanisms of immune tolerance & clinical immunity in human malaria at single cell resolution
Malaria remains a global health crisis. It causes more than 430,000 deaths a year, the majority of which are in Africa.
Children living in endemic areas are exposed to malaria parasites early in life and after 1-3 infections, if they survive, they develop immunity to the disease. However, this immunity doesn’t correspond to elimination of the parasite from their blood; instead children develop the ability to tolerate them and don’t get sick.
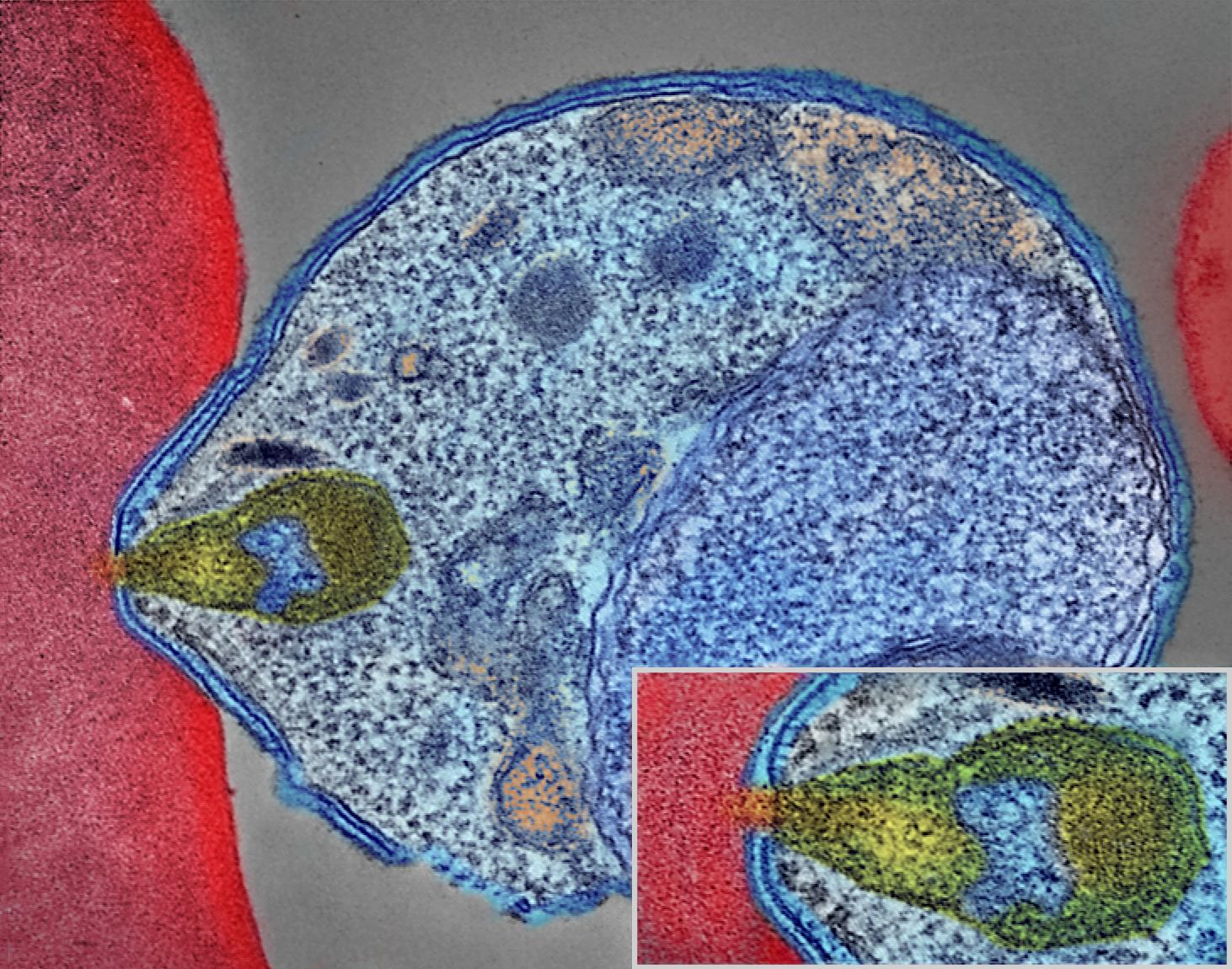
Image: NIAID [CC BY 2.0 (https://creativecommons.org/licenses/by/2.0)]
The mechanism that underpins disease tolerance in malaria is completely unknown. Understanding it will be an important tool for developing a vaccine to reduce the number of malaria deaths.
Controlled human malaria infection (CHMI) of healthy adult volunteers allows developing tolerance to be studied in a safe way – using strains of malaria that are very sensitive to available drugs – in a clinical setting. We have recently developed the first human ‘re-challenge model’, where volunteers are infected with malaria three times over a 12-month period.
Using this re-challenge study, we can find out how disease tolerance develops. Data from our pilot study (VAC063C, ClinicalTrials.gov NCT03906474) show that it’s safe for volunteers, and has revealed that a few people develop tolerance after just one infection. Our early results suggest that a type of immune cell called a T cell could be behind tolerance build-up.
In this project we want to delve a little deeper and investigate the T cells and their functions at a more detailed level, comparing first, second and third malarial infections.
Our aim is to shed light on how children adapt to tolerate malaria parasites after just three infections. In turn, this can open new avenues of research that will accelerate the design of novel anti-disease vaccines.
More about Dr Minassian here.