Respiratory syncytial virus (RSV) is a very common virus – nearly all children will catch it before they turn 2, and everyone has been infected by it several times before adulthood.
In healthy adults and older children, RSV generally causes a mild cold. Most babies only suffer from a cold too, but in about 1 in 40 cases the infection can be a lot more serious – even life-threatening. It can lead to bronchiolitis or viral pneumonia, where the lungs become congested with mucus and inflamed, causing breathing difficulties.
It’s estimated that over 30,000 babies and children under 5 are hospitalised every year in the UK because of RSV. Numbers of hospital admissions due to RSV have increased in the last 20 years, and the virus causes the deaths of around 30 babies a year in the UK. Worldwide, RSV is thought to cause about 118,000 deaths each year, and most of these are in developing countries.
There are some factors that doctors know increase the risk of babies developing a severe infection, including being exposed to tobacco smoke, being born prematurely or catching the infection under 2 months old.
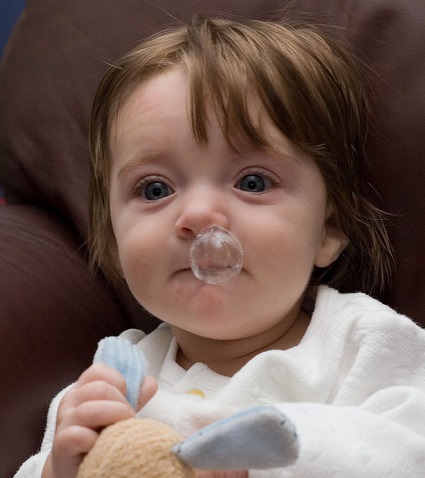
Image from
https://www.flickr.com/photos/michael_m/56454068/
But scientists don’t really know why some children become dangerously ill while most don’t. And understanding exactly what is happening to make an infection take a turn for the worst could help efforts to develop treatments or a vaccine to protect babies.
New research from Imperial College London published today in the American Journal of Respiratory and Critical Care Medicine helps shed more light on this mystery.
Which theory is right?
Scientists had two main theories as to why some babies get severely ill. Dr Ryan Thwaites, who led the research, wanted to look into these theories to find out if they were the root cause of severe infections.
“The first theory is that some babies can’t fight the virus, so it multiplies out of control. What we’d expect to see if this were the case is that babies who become severely ill have much higher levels of the virus in their nose and lungs,” says Thwaites.
“The other theory is that some babies mount a particularly powerful immune response to the virus, causing a ‘cytokine storm’”.
Cytokines are chemical messengers that orchestrate the immune system. A cytokine storm happens when the immune system overreacts to an infection, which in a respiratory infection can lead to immune cells and fluid flooding into the lungs to fight the virus, causing breathing problems.
“If this was the driving factor behind severe RSV infections, we’d expect to see high levels of cytokines like ‘interferon-gamma’ – a major culprit behind cytokine storms”, says Thwaites.
Hunting for clues
The team of researchers used gentle methods to collect samples from the noses of babies with a confirmed viral infection.
In total they collected swabs from 55 infants with bronchiolitis (34 were moderate cases, and 21 were severely ill) twice a day when possible. The process is so gentle - like putting a cotton bud into your nose - that some babies were swabbed up to 14 times.
When they compared babies who had a severe RSV infection to those with a moderate infection, they discovered that severe cases had lower viral levels and lower amounts of the cytokines linked to cytokine storms. This difference was greatest during the first week of infection.
“We were really surprised by these results,” says Thwaites. “We expected to discover severe infections to be linked to higher levels of virus and/or an overly potent immune reaction, but neither was evident in the samples we took.”
Image from
https://www.flickr.com/photos/ajc1/5497096656
When they looked at what genes were turned on and off, they found that in severe infection cases genes that control the production of a molecule called IL-17 and mucus were more active.
“This now needs more investigating, to find out what effects more IL-17 and mucus gene activation have, particularly in the lower airway, which we didn’t take samples from,” says Ryan.
If IL-17 and mucus overproduction is the root cause behind more severe infections, it could lead to new more effective treatment avenues in future.
Can human infection studies find more answers?
Due to the risk that babies can become very ill from RSV infections, it would be unethical to deliberately expose them to the virus to study their immune response in more detail.
Healthy young adults, however, only get a trifling cold (if that). Because the symptoms of an infection are so mild, there have been several research teams around the world that have carried out human infection studies (where people are purposefully given an RSV infection) to try and shine a light on the virus and why it can be so harmful.
Professor Peter Openshaw, senior researcher guiding this new study, has focussed on RSV throughout much of his career.
“We’ve been using experimental infection of adults with RSV to get a better understanding of the disease, and to test possible new treatments.
“The biggest problem with studying the immune response in adults is that it’s very different to what happens in a baby,” Openshaw says. “Their immune system is different, plus adults have been infected with RSV many times during their life. They all have pre-existing immunity.”
The only way to study RSV in babies is to collect samples from children hospitalised due to the infection. But this doesn’t capture information from babies that only experience mild symptoms as a comparison, nor uncover what happens very early in infection (before they become ill enough to receive medical care).
So what causes babies to experience severe or life-threating RSV infections is still a puzzle, and one that urgently needs solving. However, this new research provides surprising results that argue against two main current theories and provides some new avenues of research.
Emma
This research was supported by EU FP7 PREPARE and EU Innovative Medicines Initiative grant RESCEU, and Imperial’s Health Protection Research Unit (HPRU) in Respiratory Infection, the National Institute for Health Research (NIHR) Imperial Biomedical Research Centre at Imperial College Healthcare National Health Service Trust, and Pulmocide Ltd.
Ryan S. Thwaites, Matthew Coates, Kazuhiro Ito, Marwa Ghazaly, Calandra Feather, Farhana Abdulla, Tanushree Tunstall, Pooja Jain, Lindsey Cass, Garth Rapeport, Trevor T. Hansel, Simon Nadel, Peter Openshaw; Reduced Nasal Viral Load and IFN Responses in Infants with Respiratory Syncytial Virus Bronchiolitis and Respiratory Failure; American Journal of Respiratory and Critical Care Medicine; https://doi.org/10.1164/rccm.201712-2567OC